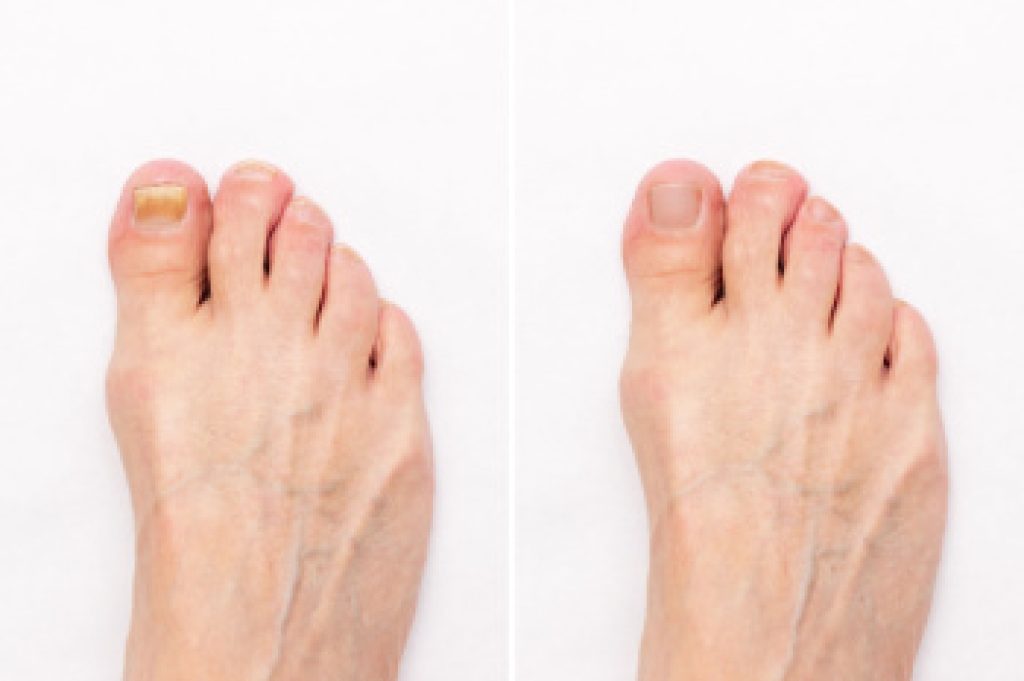
Toenail fungus, or onychomycosis, begins as a small white or yellow spot under the nail. As the fungus spreads, the nail can thicken, become discolored, and develop a brittle or crumbly texture. Without treatment, the fungus can worsen, leading to overgrowth, making it difficult to trim nails, and causing discomfort when walking. In severe cases, the nail may separate from the nail bed, increasing the risk of bacterial infection. Signs that toenail fungus is getting worse include increased nail thickening, spreading discoloration, foul odor, and pain. If left untreated, the infection can spread to surrounding skin, causing more severe issues like cellulitis. If you have signs of toenail fungus, it is suggested that you schedule an appointment with a podiatrist for a proper diagnosis and treatment.
For more information about treatment, contact one of our podiatrists of Associates in Podiatry, PC. Our doctors can provide the care you need to keep you pain-free and on your feet.
Toenail Fungus Treatment
Toenail fungus is a condition that affects many people and can be especially hard to get rid of. Fortunately, there are several methods to go about treating and avoiding it.
Antifungals & Deterrence
Oral antifungal medicine has been shown to be effective in many cases. It is important to consult with a podiatrist to determine the proper regiment for you, or potentially explore other options.
Applying foot powder on the feet and shoes helps keep the feet free of moisture and sweat.
Sandals or open toed shoes – Wearing these will allow air movement and help keep feet dry. They also expose your feet to light, which fungus cannot tolerate. Socks with moisture wicking material also help as well.
If you have any questions please contact our offices located in Pittsburgh-South Hills, and Pittsburgh-Bellevue, PA . We offer the newest diagnostic and treatment technologies for all your foot and ankle needs.